Dental bone grafting is a key procedure when there is bone loss in the jaw or maxilla, necessary for successful dental implant placement. This process seeks to restore the amount of bone lost, and it is crucial that proper post-operative care is followed to ensure proper recovery and avoid complications. Here we explain when it is necessary and how to care for the area after surgery.
What is a dental bone graft?
Dental bone grafting is a surgical procedure designed to increase the amount of bone in the jaw or maxilla, creating a solid foundation for the placement of dental implants. This procedure is essential when the bone in the desired area is insufficient to support an implant due to bone loss.
When is a dental bone graft performed?
A dental bone graft is recommended when the patient has bone loss due to causes such as:
- Periodontal diseases: Advanced periodontitis can cause significant bone loss around the teeth.
- Trauma: Accidents or injuries to the mouth can damage the jawbones.
- Use of poorly fitting dentures: Poorly fitting or long-term dentures can cause bone loss.
- Diseases such as osteoporosis or diabetes: These conditions can affect bone health, reducing jawbone density.
How is dental bone grafting performed step by step?
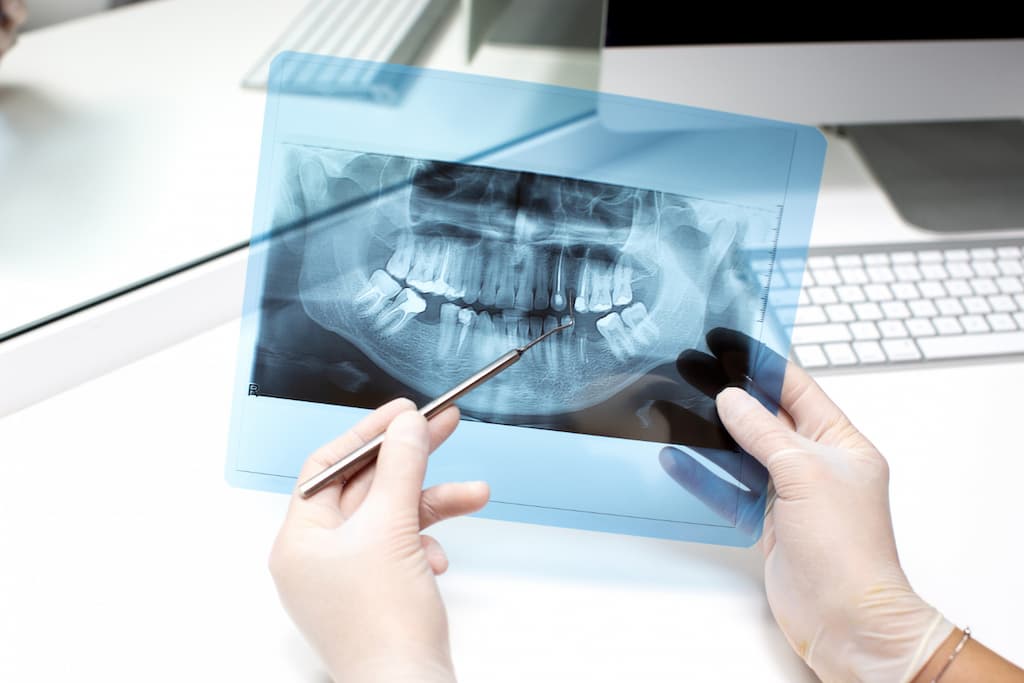
- Initial assessment and planning. Before performing the graft, the dentist or oral surgeon conducts a detailed assessment using X-rays or CT scans to determine the condition of the bone and the amount of grafting required. This planning ensures that the graft is performed in the most appropriate location.
- Selection of graft type. The selection of the type of bone graft depends on the specific situation of the patient and their needs. The main types of grafts are autogenous bone, which comes from the patient themselves, allogeneic bone, which is obtained from a donor, and synthetic or xenogeneic bone, which is of animal origin. The choice of one or the other is determined by factors such as the amount of bone needed, the patient’s overall health and their preferences, always seeking the best possible treatment outcome.
- Local anaesthesia. To ensure that the procedure is painless, local anaesthesia is administered to the area to be treated. In some cases, depending on the complexity and the patient, sedation or general anaesthesia may be used.
- Incision in the gum. Once the area is completely anaesthetised, the surgeon makes a small incision in the gum to access the area where the bone graft is required.
- Preparation of the receiving site. The surgeon prepares the affected area by cleaning and disinfecting the bone where the graft will be placed. In some cases, it is necessary to remove damaged or infected tissue before placing the graft.
- Placement of the bone graft. The bone graft is carefully placed in the prepared site. Depending on the size of the bone loss, the graft may be moulded to fit the shape of the natural bone perfectly. In some cases, membranes or additional materials may be used to ensure the stability of the graft.
- Closure of the incision. After placing the graft, the incision in the gum is closed with sutures. Sometimes, stitches are used that dissolve on their own over time.
- Initial recovery. After surgery, the patient is monitored for a short period before being allowed to go home. They are given instructions on post-operative care and possible medications, such as antibiotics and painkillers.
This procedure can take between one and two hours, depending on the complexity of the case, and is performed in a controlled clinical environment to ensure the safety and success of the graft.
Types of dental implants
There are several types of dental bone grafts, and the choice depends on the patient’s needs and the complexity of the case:
- Autogenous graft. It comes from the patient themselves, usually from the jaw, hip or tibia. It is the most effective, as it is biocompatible and has a lower risk of rejection.
- Allogeneic graft. This graft is obtained from a human donor. It is used when there is insufficient bone from the patient themselves, although it carries a higher risk of rejection compared to autogenous grafts.
- Xenogeneic graft. It comes from animals, usually cattle. Although it does not fully integrate with the patient’s bone, it serves as a scaffold that facilitates natural bone growth.
- Synthetic graft. Made from artificial materials such as hydroxyapatite or tricalcium phosphate, these grafts stimulate bone growth without risk of rejection, making them a useful option when no bone is available from the patient.
Each type of graft has its advantages and is selected based on bone availability and the patient’s specific needs.
Postoperative care for dental bone grafting
The postoperative period is crucial to ensuring the success of the graft and bone integration. Here are some key tips for proper recovery:
- Pain management. It is normal to experience discomfort during the first few days. The dentist may prescribe painkillers to manage the pain.
- Avoid physical exertion. During the first few weeks, it is important to avoid strenuous physical activity that could affect the graft.
- Proper oral hygiene. It is essential to follow your dentist’s instructions on how to brush your teeth gently to avoid damaging the graft area.
- Infection control. The dentist may prescribe antibiotics to prevent infection in the treated area.
- Gentle feeding. During the first few days, it is recommended to eat soft foods and avoid chewing in the treated area.
What to expect after the graft?
Healing of the bone graft may take several months, depending on the type of graft and the patient’s overall health. During this time, the implanted bone will integrate with the patient’s natural bone, a process known as osseointegration.
Conclusion
A dental bone graft may be necessary to ensure the success of dental implants in cases of bone loss. The post-operative period is essential for proper healing, which is why it is important to follow your dentist’s recommendations in order to achieve the best possible results. If you have any doubts or are considering this procedure, it is recommended that you consult a specialist for a personalised diagnosis.